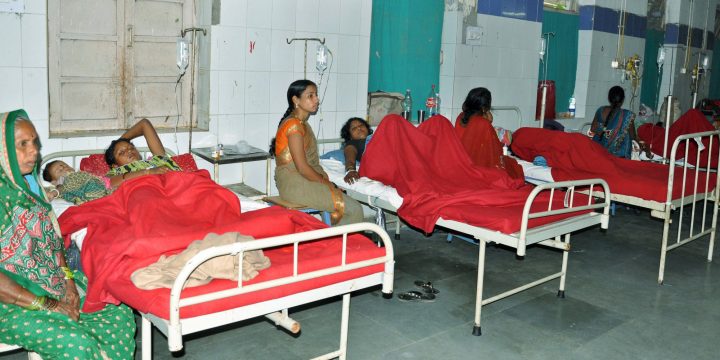
Examining India’s Changing Reproductive Health Policies
In 1952, India launched the world first national program emphasizing family planning to the extent necessary for reducing birth rates “to stabilize the population at a level consistent with the requirement of national economy”. Since then, the family planning program has evolved and the program is currently being repositioned to not only achieve population stabilization but also to promote reproductive health and reduce maternal, infant & child mortality and morbidity.
– Ministry of Health and Family Welfare, Government of India
The international community is currently debating the controversial issue of female sterilization due to a series of health policy changes in India. On one side of the issue, India officially terminated its decades-long program of sterilization camps in mid-September to the acclaim of many reproductive and maternal health advocates. On the other side, the federal government also started pilot programs for the distribution of hormonal contraceptives, which some advocates argued will potentially leave certain women at risk of forced sterilization.
On 14 September 2016, the Supreme Court of India addressed Biswas v Union of India & Ors., a public interest petition that brought the harms of the country’s long-running sterilization camps to the scrutiny of national and international actors. The Supreme Court held that these sterilization camps, which mainly affected poor rural women, presented a significant threat to the patient population and ordered the termination of these camps within three years. Critically, these camps existed under a system of corrupt incentives; sterilized individuals were formally offered a mix of money, loans, and lands while practitioners and outreach workers received compensation per patient. As such, these camps sterilized millions of patients and caused thousands of reported cases of coercion, misinformation, and substandard procedures.
The Supreme Court’s ruling followed the federal government’s announcement regarding the implementation of a DMPA program that would be freely accessible to the public. DMPA is an injectable contraceptive that reversibly affects the patient’s hormones, requiring an injection every few months to remain effective. Notably, DMPA will be the newest addition to the government’s list of reproductive health programs, which currently includes IUDs, condoms, vasectomies, laparoscopic sterilization, and oral contraceptives.
Although the WHO has strongly recommended DMPA to curb rates of maternal mortality and morbidity, various academics, public figures, and activist groups have opposed public access to the contraceptive. Many reproductive and maternal health advocates consider DMPA to be an attack on poor women because many of these patients do not have the necessary agency or information to give informed consent. For them, both the sterilization camps and the DMPA program raise similar concerns regarding women’s rights to health.
Despite this surface-level tension between the two health policy changes, both national and international actors should be pleased with the progress made to women’s maternal and reproductive health. These changes are medically safer for women. The DMPA program does not present the same population-level threat in comparison to the sterilization camps, even considering the associated health risks and the improvements to medical standards; simply, it is very unlikely that the program will cause the same level of harm. And the program is less permanent, generally allowing patients to safely conceive within a year of the last injection.
These changes are also a step towards a more just system of health care for India. Unlike the sterilization camps, there are no formal incentives that distort the patient-physician relationship. Patients do not receive anything for getting a DMPA, and healthcare workers are not rewarded a commission for performing the procedure. Admittedly, there may still exist informal, systemic factors that might negatively affect a patient’s decision; underlying issues of poverty and power tend to distort patient agency, potentially allowing coercion within this new program. But these risks are not sufficiently strong enough to justify limiting women’s access to a broader range of reproductive care alternatives. Although poor rural women will still suffer from similar distorting factors in the DMPA program that affected them in the sterilization camps, policy critiques still need to recognize and respect the positive changes in patient agency that allow for more ethical healthcare decisions. Terminating the DMPA program, as some have suggested, will simply lead to more unnecessary and unjust harm to these women.
The history of India’s sterilization camps is undeniably exploitive, and the Supreme Court’s decision to terminate the camps over the next three years was in the best interest of the public. However, health advocates should not liken the DMPA program to sterilization camps just because of superficially similar concerns regarding patient agency and informed consent. Despite the risks, which are already reduced because of advances in healthcare policies, the program could plausibly assist poor rural women by providing them with a broader range of reproductive alternatives while addressing their immediate healthcare needs. These changes in India’s health policy are imperfect; the sterilization camps could be terminated sooner, and the risks to patient agency could be further minimized. But they should nonetheless be considered positive changes for one of the world’s vulnerable populations.
(With notes from Rowena Symss.)
This article was published as part of the Osgoode chapter of Canadian Lawyers for International Human Rights (CLAIHR) media series, which aims to promote an awareness of international human rights issues.
Our website: http://claihr-osgoode.weebly.com/
Facebook: https://www.facebook.com/claihrosgoode
